Why Elbow Health Matters for Lifters
Elbow injuries affect a sizable portion of weightlifters; studies and clinical observations in the United States show that up to 5‑10 % of lifters develop medial or lateral epicondylitis (golfer’s or tennis elbow) each year. Repetitive wrist flexion, excessive grip force, and poor technique—such as locked elbows or valgus stress—place disproportionate tensile load on the medial and lateral epicondyles, leading to micro‑tears and inflammation of the forearm flexor and extensor tendons. Overloading without adequate rest compounds this stress, increasing the risk of chronic tendonopathy and even ligament injury. This article aims to explain how prevalence, mechanics, and progressive loading intersect, and to provide evidence‑based prevention and early‑intervention strategies that keep lifters training safely and sustainably.
Understanding Elbow Conditions in Lifters
Common Elbow Conditions in Lifters
| Condition | Typical Cause | Typical Symptoms | First‑line Treatment |
|---|---|---|---|
| Medial Epicondylitis (Lifter’s/ Golfer’s elbow) | Repetitive wrist flexion & gripping | Inner elbow tenderness, pain on gripping, forearm radiation | Rest, ice, compression sleeve, eccentric forearm‑flexor strengthening, brace or surgical release if refractory |
| Lateral Epicondylitis (Tennis elbow) | Repetitive wrist extension & tight grips | Outer elbow tenderness, pain with wrist extension, forearm pain | Activity modification, ice, NSAIDs, physical therapy, corticosteroid injection or surgical decompression for chronic cases |
| Olecranon Bursitis | Repeated friction or trauma to ole cranon bursa | Swelling & tenderness over the tip of the elbow | Rest, ice, compression, NSAIDs, aspiration or steroid injection if needed |
| Cubital Tunnel Syndrome | Compression of ulnar nerve at medial elbow | Numbness/tingling in ring & little fingers, weakness | Ergonomic changes, nighttime splint, nerve‑glide exercises, surgical decompression if conservative fails |
| Ulnar Collateral Ligament (UCL) injury | Overhead or throwing stresses | Deep medial elbow pain, instability | Graded loading, bracing, possible reconstruction |
 Weightlifters frequently encounter elbow pain that falls into a few well‑characterized patterns. The most common is medial epicondylitis—often called lifter’s elbow or golfer’s elbow—caused by repetitive wrist flexion and gripping. Pain is felt on the inner elbow, worsens with gripping, and may radiate down the forearm; treatment starts with rest, ice, compression sleeves, and eccentric forearm‑flexor strengthening, progressing to brace use or surgical release if needed. Lateral epicondylitis (tennis elbow) involves the extensor tendons at the outer elbow, typically from repeated wrist extension and tight grips. Management mirrors the medial form: activity modification, ice, NSAIDs, physical therapy, and, for recalcitrant cases, corticosteroid injection or surgical decompression. Outer‑elbow pain during lifts can also stem from olecranon bursitis, where fluid‑filled bursa inflames, producing swelling and tenderness; rest, ice, compression, NSAIDs, and occasional aspiration or steroid injection are effective. Cubital tunnel syndrome compresses the ulnar nerve at the inner elbow, causing numbness, tingling, and weakness in the ring and little fingers; early care includes ergonomic changes, nighttime splinting, nerve‑glide exercises, and surgical decompression if conservative measures fail. UCL injuries, more prevalent in overhead athletes, present as deep medial elbow pain and instability; they require graded loading, bracing, and possibly reconstruction. Common symptoms across these conditions include localized tenderness, pain with specific motions, swelling, and grip weakness. Dr. Rebecca S. Yu, a board‑certified orthopedic surgeon, offers comprehensive evaluation and individualized treatment plans for all five major elbow injuries encountered by lifters.
Weightlifters frequently encounter elbow pain that falls into a few well‑characterized patterns. The most common is medial epicondylitis—often called lifter’s elbow or golfer’s elbow—caused by repetitive wrist flexion and gripping. Pain is felt on the inner elbow, worsens with gripping, and may radiate down the forearm; treatment starts with rest, ice, compression sleeves, and eccentric forearm‑flexor strengthening, progressing to brace use or surgical release if needed. Lateral epicondylitis (tennis elbow) involves the extensor tendons at the outer elbow, typically from repeated wrist extension and tight grips. Management mirrors the medial form: activity modification, ice, NSAIDs, physical therapy, and, for recalcitrant cases, corticosteroid injection or surgical decompression. Outer‑elbow pain during lifts can also stem from olecranon bursitis, where fluid‑filled bursa inflames, producing swelling and tenderness; rest, ice, compression, NSAIDs, and occasional aspiration or steroid injection are effective. Cubital tunnel syndrome compresses the ulnar nerve at the inner elbow, causing numbness, tingling, and weakness in the ring and little fingers; early care includes ergonomic changes, nighttime splinting, nerve‑glide exercises, and surgical decompression if conservative measures fail. UCL injuries, more prevalent in overhead athletes, present as deep medial elbow pain and instability; they require graded loading, bracing, and possibly reconstruction. Common symptoms across these conditions include localized tenderness, pain with specific motions, swelling, and grip weakness. Dr. Rebecca S. Yu, a board‑certified orthopedic surgeon, offers comprehensive evaluation and individualized treatment plans for all five major elbow injuries encountered by lifters.
When to Seek Specialist Care and Diagnosis
Red‑Flag Symptoms & Diagnostic Pathway
| Red‑Flag Symptom | Recommended Action | Typical Imaging |
|---|---|---|
| Persistent pain > 2–3 weeks despite self‑care | Prompt orthopedic evaluation | X‑ray (bone), MRI/Ultrasound (soft tissue) |
| Sudden loss of full extension/flexion after a fall | Immediate medical attention (RICE + urgent imaging) | X‑ray ± CT (fracture/dislocation) |
| Swelling with warmth, fever | Rule out infection | Ultrasound or MRI, labs |
| Numbness/tingling + weakness | Suspect nerve compression | Nerve conduction study, MRI of elbow |
| Inability to bear weight | Possible severe ligament/ fracture injury | X‑ray, MRI, possible CT |
 Red‑flag symptoms – Persistent pain, swelling, loss of motion, numbness, tingling, or inability to bear weight after 2–3 weeks of self‑care warrants prompt evaluation. Sudden loss of full extension or flexion, especially after a fall, may indicate fracture, dislocation, or severe capsular injury.
Red‑flag symptoms – Persistent pain, swelling, loss of motion, numbness, tingling, or inability to bear weight after 2–3 weeks of self‑care warrants prompt evaluation. Sudden loss of full extension or flexion, especially after a fall, may indicate fracture, dislocation, or severe capsular injury.
Imaging studies – Initial X‑ray assesses bone alignment, joint space, and fractures. MRI or ultrasound is ordered when soft‑tissue pathology (tendon tears, ligament sprains, or nerve compression) is suspected. These modalities guide treatment decisions and rule out serious conditions such as ulnar collateral ligament rupture or osteoarthritis.
Finding a qualified orthopedic elbow specialist – Search for board‑certified orthopedic surgeons with a fellowship in elbow or upper‑extremity surgery. Use the AAOS “Find a Surgeon” directory, verify credential status, and filter by location, insurance, and patient reviews. Schedule a consultation to discuss your specific elbow problem and the surgeon’s experience with relevant procedures.
FAQ
- Finding an orthopedic elbow specialist near you: Use AAOS directory, confirm fellowship training, check insurance, and read reviews before booking.
- Inability to fully straighten the elbow: Often due to capsular contracture or arthritis; X‑ray/MRI confirms diagnosis, followed by stretching, strengthening, or arthroscopic release if needed.
- Inability to bend elbow to touch shoulder: May stem from posterior capsule tightness or scar tissue; initial therapy includes passive/active stretching and strengthening; imaging if motion does not improve.
- Inability to straighten elbow after a fall: Suggests fracture, dislocation, or ligament injury; immediate RICE, urgent X‑ray/CT, and possible surgical fixation.
- What is nursemaid's elbow?: Radial head subluxation in toddlers; treated by a simple reduction maneuver performed by a qualified clinician.
- Causes of elbow pain without injury: Overuse tendonitis, arthritis, cubital tunnel syndrome, bursitis; diagnosed via exam and imaging, then managed with activity modification, NSAIDs, and rehab.
- Elbow pain when bending and straightening: Indicates tendonitis, bursitis, or early arthritis; treated with rest, anti‑inflammatory meds, targeted stretching, and strengthening under professional guidance.
Conservative Treatment and Rehabilitation
Rehabilitation Phases for Lifter’s Elbow
| Phase | Intervention | Frequency / Duration | Primary Goal |
|---|---|---|---|
| Acute (0‑2 weeks) | RICE, NSAIDs, compression sleeve | Ice 15‑20 min 3‑4×/day | Reduce pain & swelling |
| Early (2‑6 weeks) | Gentle wrist‑flexor & extensor stretches, light isometric holds | 3×/week PT, daily home stretches | Restore ROM, begin tendon loading |
| Progressive (6‑12 weeks) | Eccentric forearm‑flexor loading (slow wrist curls, 5‑sec eccentric) | 3×/week PT, 2‑3×/day home | Tendon remodeling, strength gain |
| Return‑to‑Load (12‑24 weeks) | Gradual load increase, sport‑specific drills | Incremental 5‑10 % weekly weight rise | Full functional recovery |
| Maintenance (ongoing) | Continue eccentric program, periodic stretching | 2×/week or as needed | Prevent recurrence |
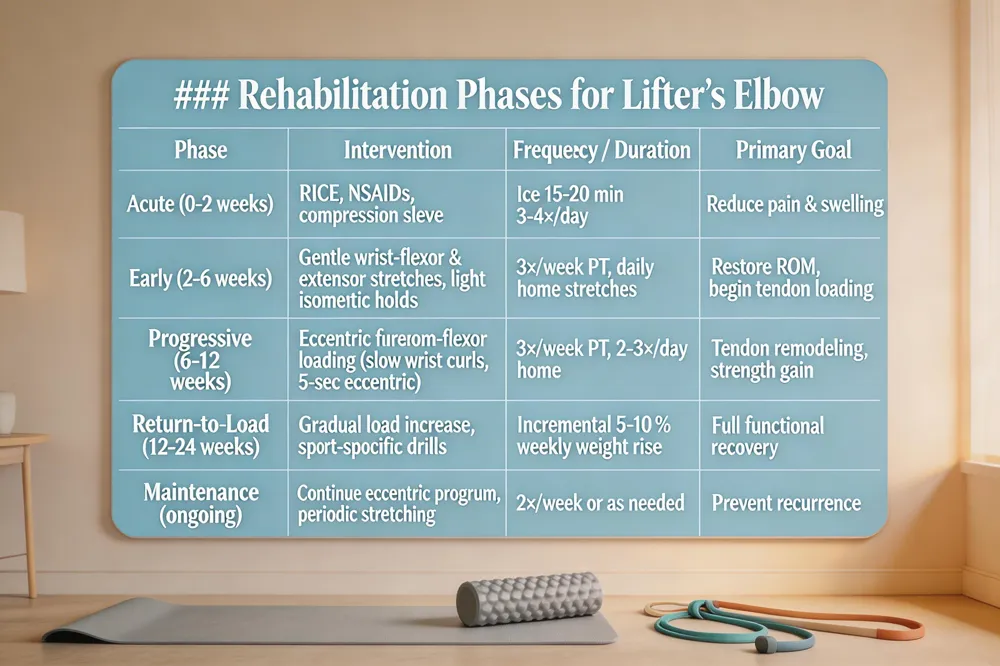 RICE protocol (Rest, Ice, Compression, Elevation) is the first line for lifter’s elbow. Apply ice for 15‑20 minutes 3‑4 times daily to reduce swelling; a compression sleeve or bandage limits excessive motion and supports the medial epicondyle. Short‑term NSAIDs such as ibuprofen or naproxen control pain and inflammation when taken as directed. Physical therapy is essential: begin with gentle wrist‑flexor and extensor stretches, then progress to eccentric loading of the forearm flexors (slow, controlled wrist curls with a 5‑second lowering phase). This promotes tendon remodeling and lowers recurrence. Recovery timelines vary—most athletes notice improvement within 6‑12 weeks, and full return to heavy lifting typically occurs in 3‑6 months if the program is followed consistently.
RICE protocol (Rest, Ice, Compression, Elevation) is the first line for lifter’s elbow. Apply ice for 15‑20 minutes 3‑4 times daily to reduce swelling; a compression sleeve or bandage limits excessive motion and supports the medial epicondyle. Short‑term NSAIDs such as ibuprofen or naproxen control pain and inflammation when taken as directed. Physical therapy is essential: begin with gentle wrist‑flexor and extensor stretches, then progress to eccentric loading of the forearm flexors (slow, controlled wrist curls with a 5‑second lowering phase). This promotes tendon remodeling and lowers recurrence. Recovery timelines vary—most athletes notice improvement within 6‑12 weeks, and full return to heavy lifting typically occurs in 3‑6 months if the program is followed consistently.
Preventing elbow injuries starts with a thorough dynamic warm‑up (arm circles, wrist rotations), proper technique, gradual load progression, and regular forearm‑strengthening work. Early discomfort should be addressed promptly with rest, ice, and stretching to avert chronic tendonitis.
To speed healing, avoid aggravating lifts, use a counter‑force brace, and adhere to the eccentric‑loading regimen. If pain persists beyond three months, options such as PRP or corticosteroid injections may be discussed with an orthopedic specialist.
Key stretches: wrist extensor (palm down, pull fingers toward forearm), wrist flexor (palm up, pull fingers back), triceps stretch (overhead elbow bend), and supinator stretch (pronated forearm rotate outward). Hold each 20‑30 seconds, repeat three times daily.
Equipment, Bracing, and Protective Strategies
Protective Gear & Usage Guidelines
| Equipment | Purpose | How to Use | Key Tips |
|---|---|---|---|
| Elbow Pad (rigid shell + cushion) | Absorb impact, protect medial epicondyle | Wear over the elbow during heavy lifts | Ensure snug fit, no restriction of ROM |
| Counter‑Force Brace (forearm strap) | Off‑load tension on flexor tendons | Position a few cm distal to elbow, tighten snugly | Wear during gripping exercises, adjust for comfort |
| Compression Sleeve | Reduce valgus strain, limit swelling | Slip over elbow, maintain moderate compression | Can be worn throughout training session |
| Wrist Rotator Band | Strengthen supinator/pronator muscles | Wrap around forearm, perform resisted rotations | Incorporate into warm‑up routine |
| Ice Pack (reusable) | Acute inflammation control | Apply 15‑20 min post‑training | Use a barrier cloth to protect skin |
 Elbow pads and sleeves are a first line of defense for lifters who experience repetitive strain or post‑injury swelling. A well‑designed pad combines a rigid outer shell for impact absorption with a cushioned inner layer that conforms to the joint, allowing full range of motion while protecting the medial epicondyle from direct blows. Counter‑force braces (forearm straps) work by applying pressure just distal to the elbow, off‑loading tension on the flexor tendons that cause medial epicondylitis. Proper sizing and placement are essential; Dr. Yu advises that the strap sit snugly, a few centimeters below the elbow and be worn during heavy gripping activities. For general support, a soft compression sleeve can reduce valgus strain without restricting movement. Maintaining a neutral wrist alignment and a firm but not excessive grip during presses, rows, and curls minimizes torque on the medial epicondyle. A preventive warm‑up should include dynamic forearm stretches, wrist rotations, and light resistance band work for 5‑10 minutes before lifting. Ice therapy (15‑20 minutes) after training, NSAIDs for acute inflammation, and a gradual return to load with eccentric forearm strengthening further relieve pain. If discomfort persists, Dr. Yu recommends a professional evaluation to tailor bracing and rehabilitation to the specific elbow condition.
Elbow pads and sleeves are a first line of defense for lifters who experience repetitive strain or post‑injury swelling. A well‑designed pad combines a rigid outer shell for impact absorption with a cushioned inner layer that conforms to the joint, allowing full range of motion while protecting the medial epicondyle from direct blows. Counter‑force braces (forearm straps) work by applying pressure just distal to the elbow, off‑loading tension on the flexor tendons that cause medial epicondylitis. Proper sizing and placement are essential; Dr. Yu advises that the strap sit snugly, a few centimeters below the elbow and be worn during heavy gripping activities. For general support, a soft compression sleeve can reduce valgus strain without restricting movement. Maintaining a neutral wrist alignment and a firm but not excessive grip during presses, rows, and curls minimizes torque on the medial epicondyle. A preventive warm‑up should include dynamic forearm stretches, wrist rotations, and light resistance band work for 5‑10 minutes before lifting. Ice therapy (15‑20 minutes) after training, NSAIDs for acute inflammation, and a gradual return to load with eccentric forearm strengthening further relieve pain. If discomfort persists, Dr. Yu recommends a professional evaluation to tailor bracing and rehabilitation to the specific elbow condition.
Return to Training and Long‑Term Joint Health
Return‑to‑Training Guidelines & Long‑Term Health
| Recommendation | Details | Frequency / Notes |
|---|---|---|
| Load Progression | Increase weight ≤ 5‑10 % per week | Monitor pain, stop if symptoms recur |
| Rest Intervals | Minimum 48 h between intense elbow sessions | Supports collagen synthesis |
| Cross‑Training | Alternate grip positions, use lower‑body/cardio days | Reduces repetitive stress |
| Nutrition | 1.2‑1.6 g protein/kg body weight, vitamin C, omega‑3 | Daily intake for tendon healing |
| Hydration & Anti‑Inflammatory Diet | Adequate water, limit processed foods | Daily habit |
| Early Overuse Signs | Dull ache, localized tenderness, grip weakness | Reduce volume immediately, resume stretching |
| Periodic Re‑Evaluation | Follow‑up with orthopedic specialist if pain > 3 months | Adjust rehab program as needed |
 A gradual return to weightlifting is essential for preventing re‑injury. Begin with light loads, keep the wrist neutral, and use a controlled grip. Increase weight by no more than 5‑10 % each week while watching for any return of pain. Adequate rest days are equally important; tendons remodel more slowly than muscle, so at least 48 hours of recovery after intense elbow‑loading sessions supports collagen synthesis and tissue repair.
A gradual return to weightlifting is essential for preventing re‑injury. Begin with light loads, keep the wrist neutral, and use a controlled grip. Increase weight by no more than 5‑10 % each week while watching for any return of pain. Adequate rest days are equally important; tendons remodel more slowly than muscle, so at least 48 hours of recovery after intense elbow‑loading sessions supports collagen synthesis and tissue repair.
Cross‑training and varying exercise selection reduce repetitive stress on the medial elbow. Alternate movement patterns, use different grip positions, and incorporate lower‑body or cardio sessions to give forearm flexors time to recover. Early signs of overuse—dull ache at the end of range, localized tenderness, and reduced grip strength—should trigger immediate volume reduction and targeted stretching to stop progression to chronic tendinopathy.
Nutrition plays a pivotal role in tendon healing. Aim for 1.2–1.6 g protein per kilogram body weight daily, and include vitamin C and omega‑3 fatty acids to stimulate collagen formation. Proper hydration and limiting processed foods lower systemic inflammation, further supporting tissue repair.
Take Control of Your Elbow Health Today
Preventing lifter’s elbow starts with a thorough warm‑up that includes dynamic forearm, wrist and shoulder stretches, followed by progressive loading and adequate rest days. Keep the wrist neutral, avoid excessive grip force, and use supportive gear such as elbow sleeves or wrist wraps. Ice the elbow 15‑20 minutes after each session, and consider short‑term NSAIDs for pain control. Early intervention with gentle stretching and eccentric strengthening of the forearm flexors and extensors promotes tendon resilience. If pain persists beyond a few weeks, seek evaluation from a board‑certified orthopedic specialist who can design a personalized rehabilitation plan. Book your appointment today to protect your elbows and stay strong and achieve peak performance safely daily.
